Trauma Symptoms: Emotional, Physical, and Relational Signs
There are a lot of examples of what trauma can look like in shows and movies, but trauma doesn’t always look that way, or even the way we expect it to. Many adults associate trauma with a single, catastrophic event—an accident, an assault, or a natural disaster. While these experiences absolutely can be traumatic, trauma can also develop from other life factors one may not always consider, like chronic stress, emotionally unsafe relationships, childhood neglect, medical complications, systemic oppression, or repeated experiences of not feeling seen, protected, or supported.
Especially when trauma is a result of some of these ongoing life factors, it shows up less as a clear memory of what happened and more as ongoing symptoms in the body, dysregulated emotions, and rocky relationships. When experiencing trauma symptoms, an adult might feel like they’re overreacting to minor situations, disconnected from others or themselves, chronically exhausted, or stuck in patterns they can’t seem to change—without fully understanding why.
Below, we explore common trauma symptoms in adults, how they differ from anxiety or depression, and when it may be time to seek trauma-informed therapy.
Emotional Symptoms of Trauma
Trauma significantly impacts the nervous system and the brain’s threat-detection system. When the body has learned that the world is unpredictable or unsafe, emotions can feel intense, muted, or confusing.
Anxiety and Hypervigilance
Many adults with trauma experience chronic anxiety, even when life appears relatively stable. This anxiety may not be tied to a specific fear, but rather a constant sense of unease or anticipation that something bad is about to happen.
Symptoms can include:
Racing thoughts
Difficulty relaxing or feeling “on edge”
Heightened startle response
Trouble sleeping or frequent nightmares
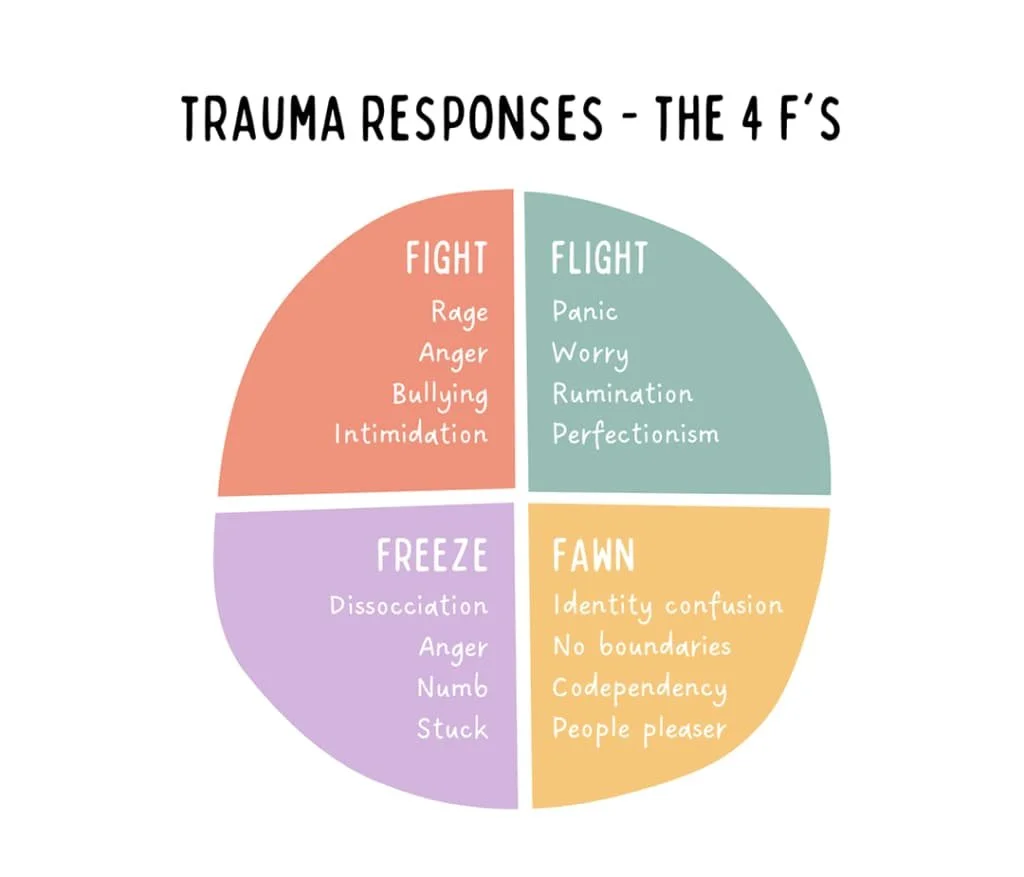
This is often a sign of hypervigilance—the nervous system remaining in a fight-or-flight state long after a threat has passed.
Emotional Numbness or Disconnection
Not all trauma responses involve heightened emotion. Alternatively, trauma can lead to emotional numbness or feeling shut down. This can feel like emptiness, detachment, or going through life on autopilot.
Emotional numbing may include:
Feeling disconnected from yourself or others
Lacking empathy
Difficulty accessing joy, sadness, or excitement
A sense of unreality or feeling "far away" from your life
Trouble identifying or naming emotions
This response is the nervous system’s way of protecting you from overwhelm, especially if emotions once felt unsafe.
Shame and Self-Blame
Shame and self-blame are two of the most common emotional symptoms of trauma. Rather than viewing the traumatic experience as something that happened to you, trauma can lead to deeply ingrained beliefs such as:
“Something is wrong with me.”
“I’m too much.”
“I should have known better.”
“I brought this on myself.”
These beliefs often develop early and aren’t always conscious thoughts, making them hard to identify. Yet, they can negatively shape self-esteem, decision-making, and relationships.
Physical Symptoms of Trauma
Trauma is not just stored in the mind; it lives in the body. When the body’s stress response (i.e. “fight-or-flight”) remains activated for long periods of time, it can contribute to a wide range of physical symptoms. These physical symptoms are often psychosomatic, meaning they do not have a clear medical explanation. With that being said, it’s not “all in your head.” These symptoms are very real, they are simply a result of the trauma, rather than originating from any physical, medical concern.
Chronic Pain and Tension
Many adults with trauma experience ongoing muscle tension, headaches, jaw pain, neck or back pain, or generalized body aches. This is due to the body bracing against perceived threats, even during rest or when there are no real threats present.
This non-stop tension can lead to chronic pain. The human body is designed to create tension in temporary bursts, as a means to protect against physical and emotional threats. However, when this tension becomes chronic, rather than temporary, it can have lasting effects on one’s tolerance to pain and overall physical functioning.
Gastrointestinal Issues
The gut and nervous system are closely connected. Due to this close relationship, trauma can disrupt the nervous system, and in turn, impact digestion. This can contribute to:
IBS, with constipation or diarrhea
Chronic stomach pain or nausea
Appetite changes
Bloating
While these stress-related gastrointestinal symptoms can occur regularly, the symptoms often worsen during heightened emotional distress or relational conflict, and diminish or cease altogether during times of rest and relaxation.
Fatigue and Burnout
Living in a prolonged state of survival is exhausting. Trauma-related fatigue can look like:
Feeling tired no matter how much you rest
Difficulty getting out of bed
Brain fog or trouble concentrating
Frequent illness or weakened immunity
This fatigue is not laziness. It is the cost of a nervous system that has been working overtime for months or years.
Behavioral Patterns Linked to Trauma
Trauma often shapes behavior in subtle but powerful ways. These patterns once served a protective purpose, even if they now feel limiting or frustrating.
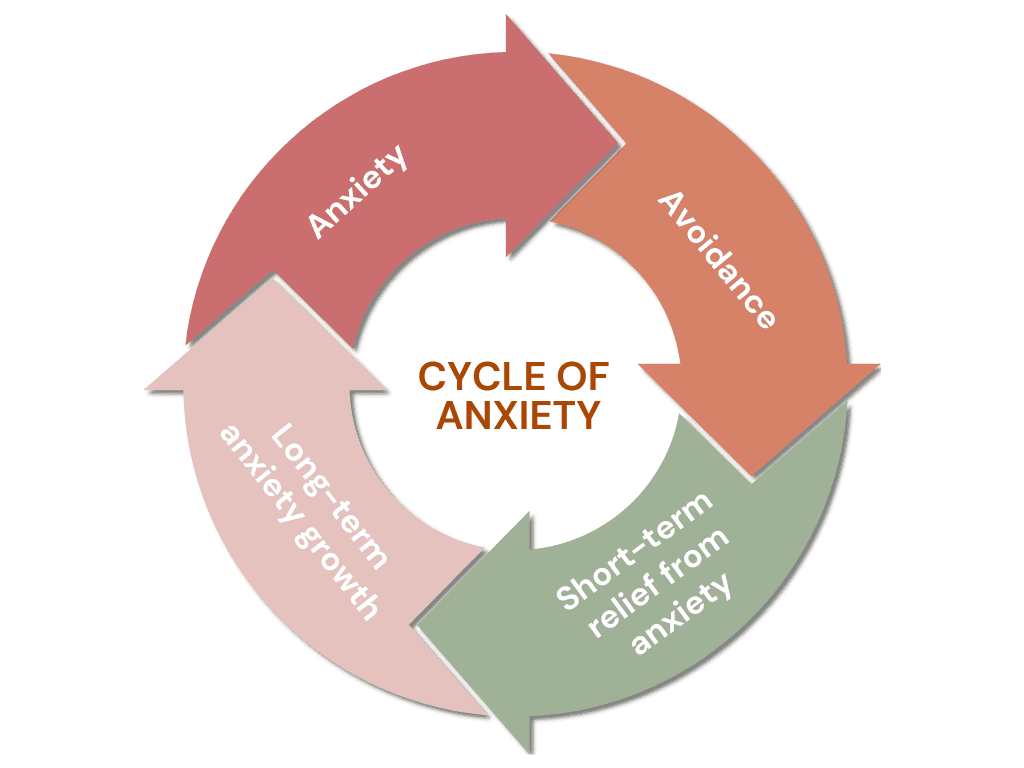
Avoidance
Avoidance is a core trauma response. This might include avoiding:
Certain places, people, or conversations
Conflict
Emotional intimacy
Memories
Feelings
Bodily sensations
While avoidance can bring short-term relief, it often reinforces anxiety and keeps trauma symptoms stuck.
People-Pleasing
Many adults with relational or developmental trauma learn that safety comes from being agreeable, helpful, or easy to be around.
People-pleasing patterns may involve:
Difficulty saying no or setting boundaries
Prioritizing others’ needs over your own
Fear of disappointing or upsetting others
Losing touch with your own wants and needs
Perfectionism and Over-Functioning
Perfectionism can be a trauma response rooted in control. If mistakes once led to criticism, rejection, or danger, the nervous system may equate being flawless with being safe.
This can show up as:
Chronic self-criticism
Overworking or overachieving
Fear of failure
Guilt at rest or when not being “productive”
Difficulty delegating or trusting others
Relationship and Attachment Patterns
Trauma—especially developmental or relational trauma—often impacts how adults connect to others. Adults with trauma may experience insecure attachment patterns, such as:
Anxious attachment: An individual has a fear of abandonment, heightened sensitivity to rejection, and often seeks reassurance as a means to reduce anxiety.
Avoidant attachment: An individual engages in emotional distancing, has discomfort with vulnerability, and is self-reliant to a fault.
Disorganized attachment: An individual experiences the push-pull dynamic of wanting closeness but fearing it at the same time.
These patterns are developed in response to traumatic experiences. They are learned strategies for navigating connections when safety felt uncertain, and continue to persist long after the trauma or threat has subsided.
Trauma can contribute to various interpersonal challenges, such as difficulty trusting others, intense reactions to perceived rejection, repeated cycles of unhealthy relationships, conflict avoidance or explosive conflict, and feeling chronically unseen or misunderstood. Because of these relational patterns, treating trauma often involves healing within relationships, both in therapy and in safe, supportive connections.
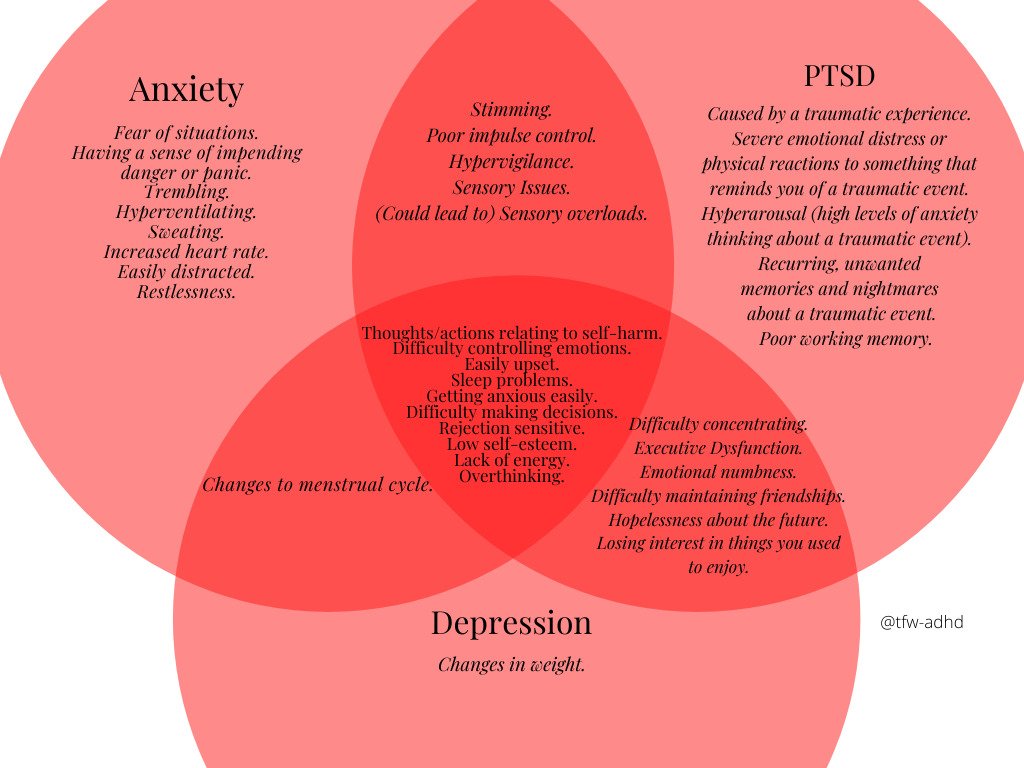
Trauma vs. Anxiety vs. Depression
Trauma symptoms can overlap with anxiety and depression, which is why trauma is sometimes misdiagnosed or overlooked. Anxiety is often defined by future-oriented worry and behaviors driven by fear. Depression, in contrast, typically focuses on thoughts of the past which influence low mood, hopelessness for the future, and a loss of interest in daily activities. While anxiety and depression can exist on their own, they are also common outcomes of unresolved trauma. Treating trauma often reduces anxiety and depressive symptoms at their core.
When Trauma Symptoms Signal It’s Time to Seek Therapy
You don’t need to have a clear trauma story, or feel “bad enough,” to benefit from trauma therapy. It may be time to seek support if your symptoms are interfering with daily life, work, or relationships, you feel stuck in patterns you intellectually understand but can’t change, your body feels constantly tense, exhausted, or unsafe, you’ve tried traditional coping strategies without lasting relief, or you suspect your reactions are tied to past experiences.
It’s important to note that trauma-informed therapy doesn’t have to focus on reliving or forcing memories of the trauma experienced. Instead, it focuses on safety, nervous system regulation, connection, and compassion. Different types of therapy, such as EMDR, Internal Family Systems (IFS), somatic therapy, and attachment-based approaches help adults heal at both the emotional and physiological level.
Trauma symptoms are not signs of weakness. They are evidence of a nervous system that adapted to survive. With the right support, it is possible to feel more grounded, connected, and at ease in your body and relationships.
If you recognize yourself in any of these patterns, you are not alone—and you don’t have to navigate healing on your own. Trauma therapy can help you move from survival into a life that feels safer, fuller, and more aligned with who you truly are.